Skin marking
Influenced by gender, race, and unique facial features of each patient:
- Gender
- In women, the brow and lid creases are higher and more arched, and the lid fold is less prominent.
- In men, the brow protrudes more anteriorly, and the eyelid crease is closer to the eyelid margin.
- Age
- Younger patients may want to retain fullness above the lid crease so that preservation of orbicularis muscle may be considered
- Older patients may need to retain blink efficiency so that so that preservation of orbicularis muscle may be considered
- Race
- In Caucasian women, the crease is usually 8–11 mm above the lid margin
- In Caucasian men, the crease is usually 6–9 mm above the eyelid margin.
- The Asian upper eyelid has more fullness, narrower palpebral fissures, more prominent medial epicanthal folds, and a lid crease closer to the eyelid margin.
- Lid crease in Asians can be absent, may be nasally tapered, or flat but typically lies lower and flatter than Caucasians.
- In Caucasians, the orbital septum attaches to the levator aponeurosis at or slightly above the superior tarsal border or over the anterior surface of the tarsus.
- In Asians, the orbital septum fuses to the levator aponeurosis at variable distances below the superior tarsal border
- Preaponeurotic fat pad protrusion and a thick subcutaneous fat layer prevent levator fibers from extending toward the skin near the superior tarsal border
- The primary insertion of the levator aponeurosis into the orbicularis muscle and into the upper eyelid skin occurs closer to the eyelid margin in Asians.
- Asian eyelid includes a pretarsal fat pad and may include more volume in the preaponeurotic fat pads.
- Unique facial features
- Patients may prefer to retain or change certain features such as relative hollowness or fullness of the upper eyelid sulcus. Removal or preservation of fat and muscle can help achieve these goals. Review of old or family photographs may be helpful in clarifying preferences and objectives.
- One approach to assuring that sufficient skin remains for complete closure of the eyelid is the 20‑mm rule.
- A total of 20 mm of skin should remain when measured vertically between the lower margin of the central eyebrow and the margin of the central eyelashes.
- If the lid crease is marked 8 mm above the lash margin, for example, the upper edge of the incision should be 12 mm below the brow margin.
- An alternative approach is the "pinch method" where eyelid skin is grasped and gathered until the skin is tight and the lashes begin to evert.
- The eyelid crease may be between 4–12 mm above the lash line.
- In Asians, the lid crease is usually 4–6 mm above the lash margin
- In Caucasians, usually 8–10 mm above the lash margin
- The lower lateral marking is extended to the orbital rim or end of the eyebrow and may course superiorly or follow existing creases to meet the upper mark.
- Extending the marking too far lateral may result in unwanted visible scarring.
- However with skin closure, this scar generally blends well with the normal smile lines in the lateral canthal area.
- After marking is complete and before injection of local anesthetic, the lack of skin elasticity may make the marks look irregular and malpositioned.
Injection of local anesthetic
- Timing
- May be administered in the operating room or preoperative holding area
- Early injection takes advantage of the time required to move, position, prep, and drape the patient, during which time the anesthetic will take effect.
- Dosing
- 1% or 2% lidocaine with 1:100,000–200,000 units of epinephrine is typically used, sometimes with the addition of hyaluronidase.
- Approximately 1–1.5 cc of anesthetic is injected through a 27- or 30‑gauge needle in the plane between skin and orbicularis muscle across the entire eyelid.
- Great care is taken to point the needle away from the globe, to avoid inadvertent penetration with sudden patient movement.
- In lidocaine (amide-type) sensitive patients, procaine (ester-type) may be used.
- The addition of epinephrine to local anesthetic solutions prolongs the duration of action of the anesthetic agent and may reduce intraoperative bleeding.
- The alternative argument is that epinephrine vasoconstriction is followed by rebound vasodilation, which may actually potentiate the risk of postoperative orbital hemorrhage.
- Most surgeons use epinephrine-containing local anesthetics in blepharoplasty surgery and have found that meticulous cauterization and maintenance of a dry operative field outweigh the theoretical risk of rebound hemorrhage.
Tissue excision
- Some surgeons prefer to place a corneal protector in each eye.
- This is particularly important if incisions are made with the CO2 laser.
- The incision, which is made along the previously marked lines, can be made with a 15 Bard Parker blade, an incisional CO2 laser, a diamond blade, or a needle-tipped Bovie or radiofrequency instrument.
- Depth of excision depends on the preoperative plan.
- Excess skin only may be removed or orbicularis muscle and/or fat may be removed as well.
- Partial removal of orbicularis over the lateral orbital rim area may provide a small eyebrow elevation.
- Partial removal of orbicularis muscle over the medial eyelid area with grafting of medial fat into the lateral sub-brow area has been proposed to restore youthful contours (Fezza J, OPRS 2012;28:446).
- The tissue to be excised is grasped with a forceps and meticulously dissected along the intended plane.
- Cautery is applied as needed to achieve hemostasis.
- Excess preaponeurotic and/or nasal fat is removed.
- Care is taken not to remove too much of this volume producing tissue, particularly in the pupillary meridian where inadequate fat will often cause an A‑frame deformity.
- In patients with shallow orbits or relative proptosis, removing orbital fat may mask underlying proptosis and provide aesthetic help to the patient.
- Alternatively, removing anterior fat may unmask the underlying proptosis, and care should be exercised.
- If the nasal fat pad fat is to be removed, care is taken to cauterize or avoid medial palpebral vessels which course over the medial fat pad.
- Gentle cautery applied to the orbital fat may contour and replace the remaining fat posteriorly into the orbit, providing needed volume and fullness.
- Care is taken to avoid the levator palpebrae superioris complex which lies just posterior to the preaponeurotic fat pad.
Wound closure
- In addition to primary closure of the skin, attention may focus on creation of symmetric and well-positioned eyelid creases.
- Lid crease fixation is not always necessary.
- When needed, lid crease fixation method depends on surgeon's preferences and experience (Video 1).
- Interrupted suture placement can incorporate superficial fibers of levator aponeurosis just above the superior edge of the tarsal plate.
- Absorbable subcutaneous suture such as 7‑0 polyglactin can be placed, anchoring superficial levator fibers to the overlying skin.
- Running, interrupted, subcuticular, and other cutaneous skin closures can be with absorbable or nonabsorbable suture, incorporating skin and orbicularis muscle tissue, which aids in the lid crease formation (Video 2).
- As an alternative to suture closure, some surgeons prefer octyl‑2‑cyanoacrylate for blepharoplasty wound closure.
- Temporary sutures may approximate the skin before application of the glue.
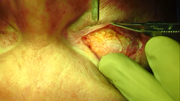
Video 1. Laser can be used to expose the superficial fibers of the levator for incorporation into the skin closure.
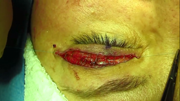
Video 2. Subcuticular closure.
Wound care
- Antibiotic ointment may be placed over incision.
- Moistened gauze may be placed over the closed eyelids.
- Many surgeons apply a cold compress while the patient is in the recovery area.
- Before discharge, wounds are checked for bleeding and dehiscence.